Do I Need an Injection for a Prolapsed (Slipped) Lumbar Disc?
If you’ve been diagnosed with a prolapsed (slipped) lumbar disc, you may hear or read about spinal injections. A common and understandable question is:
“Do I really need an injection?”
The short answer is: Not always.
Injections can be helpful in selected cases — but they are not required for everyone.
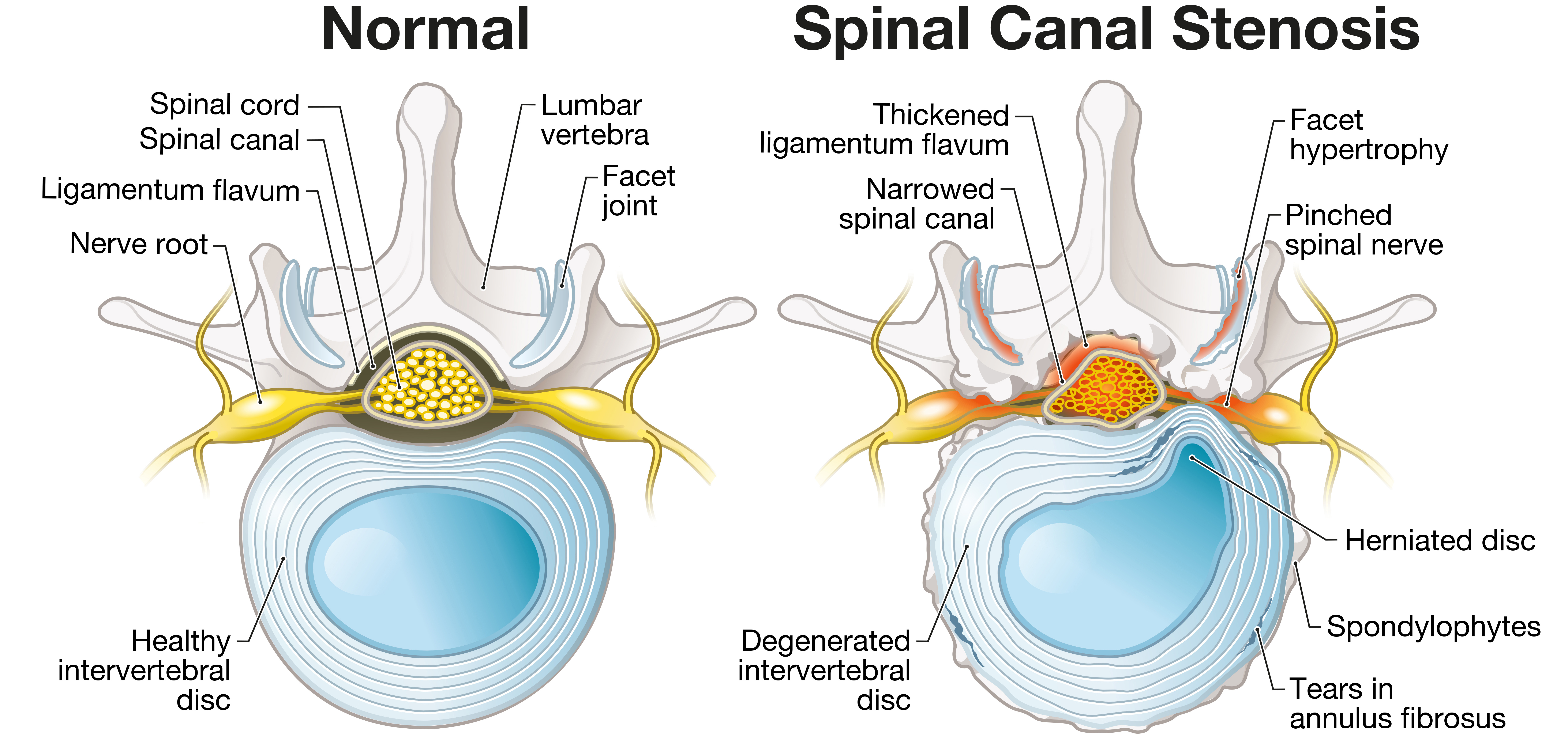
What Is a Prolapsed Lumbar Disc?
A prolapsed lumbar disc (also called a herniated or slipped disc) occurs when part of a disc in the lower back bulges or protrudes and irritates a nearby nerve.
This often causes:
- Lower back pain
- Sciatica (leg pain travelling down from the back)
- Numbness or tingling
- Occasionally weakness in the leg
Importantly, most prolapsed discs improve naturally over time.
Why Are Injections Recommended?
The leg pain associated with a prolapsed disc is usually caused by inflammation around the nerve, not simply pressure.
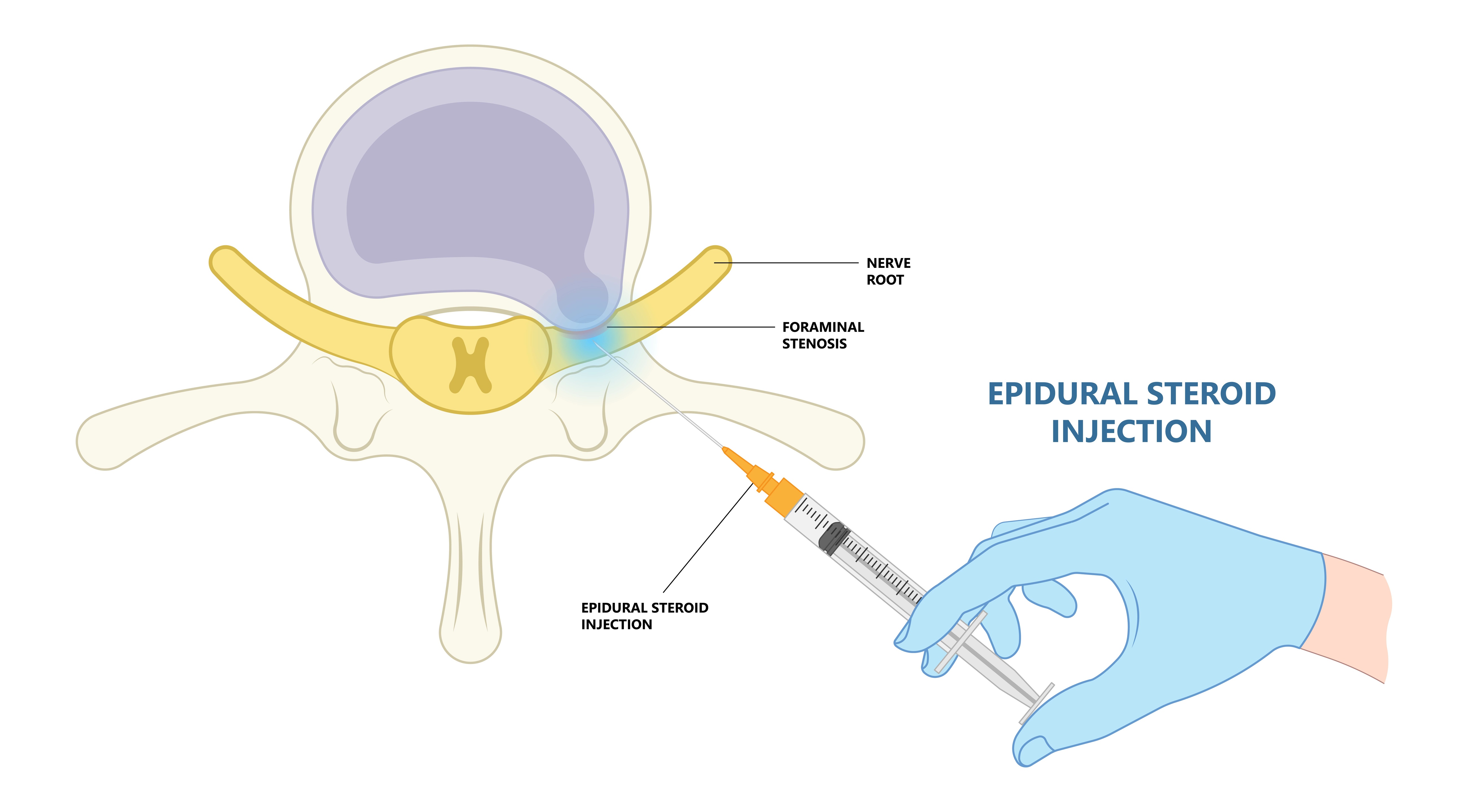
An injection — typically an epidural steroid injection or nerve root injection — aims to:
- Reduce inflammation
- Relieve leg pain
- Allow improved mobility
- Facilitate rehabilitation
It does not push the disc back into place.
It is designed to calm the irritated nerve.
Do All Patients with a Prolapsed Disc Need an Injection?
No.
Approximately:
- 75% of patients experience improvement in lumbar sciatica symptoms within 3 months of onset
- Up to 90% improve within 4 months with conservative management
Many patients improve with:
- Time
- Physiotherapy
- Sensible activity modification
- Pain management
An injection is usually considered when:
- Leg pain remains significant after several weeks
- Pain is limiting work or sleep
- Physiotherapy is difficult due to pain
- There is a need to reduce reliance on strong pain medication
It is not routinely required for mild or improving symptoms.
How Effective Are Lumbar Disc Injections?
Research shows that spinal injections:
- Can provide short- to medium-term pain relief
- Are most effective for leg pain (sciatica)
- May reduce the need for surgery in some patients
Relief may last weeks to several months.
Approximately 66% to 75% of patients with lumbar sciatica experience improvement after epidural steroid injections, defined as at least 50% pain relief or a positive global perceived effect at 1 month.
They are generally less effective for isolated lower back pain.
Do Spinal Injections Cure a Prolapsed Disc?
No.
Spinal injections do not “push the disc back in” or remove the prolapse.
They reduce inflammation around the nerve, which can significantly improve pain and mobility. In many cases, this allows the body time to heal naturally.
When Is an Injection Not Appropriate?
An injection may not be recommended if:
- Symptoms are mild and improving
- Pain is mainly in the lower back rather than the leg
- There is significant leg weakness (where surgery may be more appropriate)
- Symptoms have resolved
Careful clinical assessment is essential before proceeding.
Does Needing an Injection Mean Surgery Is Inevitable?
No.
In many cases, an injection is used to:
- Provide pain relief
- Allow the body time to heal
- Support physiotherapy
- Avoid or delay surgery
Most prolapsed lumbar discs settle over time.
Surgery is typically reserved for:
- Persistent severe leg pain
- Progressive weakness
- Failure of conservative treatment
Are Lumbar Injections Painful?
Most injections are performed under local anaesthetic and imaging guidance.
You may feel temporary pressure or mild discomfort, but the procedure is usually well tolerated. Some patients experience temporary soreness for a day or two afterwards.
How Long Does Pain Relief Last?
Relief varies between individuals.
- Some patients experience improvement for several weeks
- Others may have relief lasting several months
- Occasionally, symptoms return gradually
Some patients need only one injection; others may require further treatment.
Are Lumbar Injections Safe?
When performed under imaging guidance by an experienced specialist, spinal injections are generally safe.
Temporary side effects may include:
- Soreness at the injection site
- Temporary increase in pain
- Facial flushing
Serious complications are uncommon. Your spinal specialist will discuss the procedure and associated risks with you.
Blood-thinning medications may need to be stopped before the injection (under medical guidance).
Key Takeaway
You do not automatically need an injection simply because you have a prolapsed lumbar disc.
Many patients recover with conservative treatment alone.
An injection may be helpful if leg pain remains significant and is limiting recovery — but it should be part of a structured, evidence-based treatment plan.
The goal is always the same:
To relieve pain, restore movement, and avoid unnecessary intervention wherever possible.
If you are experiencing persistent leg pain or have been advised to consider a spinal injection, a specialist assessment can help determine the most appropriate course of treatment.
Consultant-led spine care is available, with a focus on clear diagnosis, evidence-based management, and recommending intervention only when truly indicated.
Appointments:
📧 contactspinecare.uk@gmail.com
📞 07771112322

.png)