Cervical Laminectomy
What is Cervical Laminectomy?
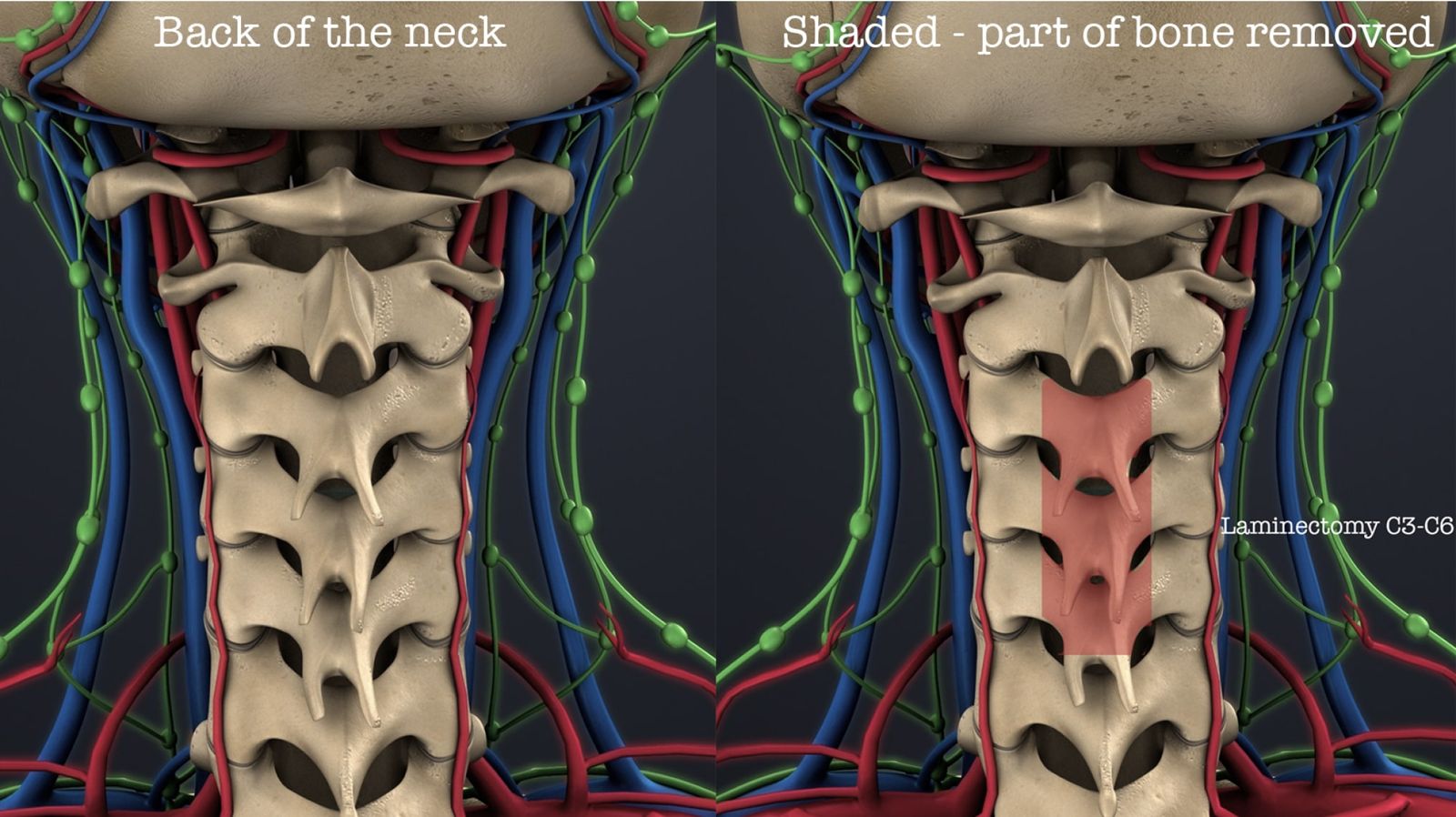
Cervical Laminectomy is a surgical procedure involving removing part of the neck vertebral bone called the lamina.
The lamina is a flat, thin vertebral arch component covering the spinal cord and nerves found in the back of the neck.
Why is it done?
Generally, cervical laminectomy is carried out to ease the pressure on the spinal cord that results from conditions like spinal stenosis, spinal tumours, or herniated discs.
The narrowing of the spinal canal can compress the spinal cord and nerves, such as weakness, numbness, and tingling sensations in the arms and legs, problems with balance and coordination, and bladder or bowel dysfunction. The severity of these symptoms depends on the extent of the stenosis.
The primary objective of surgery is to eliminate pressure on the spinal cord and avoid further damage to the area.
However, the results can vary depending on the extent of the initial damage. Patients who receive surgery before severe damage has occurred typically have the best outcomes.
Following the procedure, some patients may experience partial restoration of spinal cord function, moderate improvements in hand function and walking ability, and partial sensation in their hands.
If a significant amount of numbness existed prior to surgery, it might not completely dissipate. While relief from arm pain is probable, it’s uncertain whether neck pain will improve. Consequently, cervical decompression surgery is not typically performed for individuals who experience neck pain alone without other symptoms. If the surgery prevents additional spinal cord damage and does not result in loss of function, both the patient and surgeon should consider it a success.
What happens during the procedure?
Before the procedure, the patient will typically undergo a thorough evaluation by the surgeon to determine the underlying cause of their pain and whether a cervical laminectomy is an appropriate treatment option. This will also include an anaesthetic assessment for fitness for surgery.
The surgery is usually performed under general anaesthesia, and the patient lies face down on the operating table.
The surgeon makes a midline incision in the lower back over the affected area.
The surgeon then uses a microscope/ surgical loupes and specialized instruments to remove the portion of the disc that is compressing the spinal nerves. Magnification has its advantages like enhanced visualisation, improved precision, reduced trauma, and quicker recovery (reduced trauma and small incisions).
Surgery aims to remove the material (for example, the excess bone and ‘thickened’ ligament) from the back of the spinal canal to give the spinal cord more room.
Sometimes, the cervical spine is fused at two or more vertebrae together using bone grafts, screws, and rods.
The procedure typically takes one or more hours, depending on the extent of the stenosis and the case’s complexity.
What happens after the procedure?
After the procedure, the patient is taken to a recovery room, where they are monitored briefly before discharge. Patients can usually return home after safely mobilising following the surgery. Depending on the case’s complexity, this may be a day or a couple of days.
Pain is common after cervical laminectomy surgery. Patients are given pain medications to manage the discomfort. Patients may be advised to wear a neck brace for several weeks after surgery. They may also be instructed to avoid bending, lifting, or twisting their neck for several weeks. Patients may need to undergo physical therapy to strengthen their neck muscles and improve their range of motion. The recovery period varies for each patient, but most people can return to work within 2-6 weeks after surgery, depending on the nature of their job.
If necessary, physical therapy is typically initiated after the surgery to enhance the patient’s strength and flexibility.
What are the potential side effects of the procedure?
As with any form of surgery, there are risks associated with it. These are nerve root damage, spinal cord damage, dural tear, recurrence, bleeding, infection, ongoing pain, blood clots in legs/lungs, non-union, stroke, heart attack, medical or anaesthetic problems or death.
These risks and benefits will be discussed in detail during the consent process.
Please follow the BASS (British Association of Spinal Surgeons) website for more information.
Learn more about condition:
Cervical Disc Myelopathy: Explore the causes and symptoms associated with Cervical Disc Myelopathy.